Important: This article provides educational information only. Treatment decisions should always be made in consultation with qualified mental health professionals who can evaluate your specific situation.
If you’re living with treatment-resistant depression, you may be considering advanced brain stimulation therapies such as TMS or ECT. Many patients researching TMS compared to ECT want to understand which option may fit their needs best.
Both are FDA-approved and effective, but they differ significantly in how they are delivered and tolerated.
In many non-emergency cases, TMS is recommended as the best initial treatment because it does not require anesthesia, has a lower risk of cognitive side effects, and allows patients to maintain their daily responsibilities. ECT remains highly effective and is typically reserved for severe, urgent, or life-threatening depression where rapid symptom relief is critical.
What Makes TMS and ECT Different?
TMS and ECT both treat depression by changing how the brain works, but they do it in very different ways.
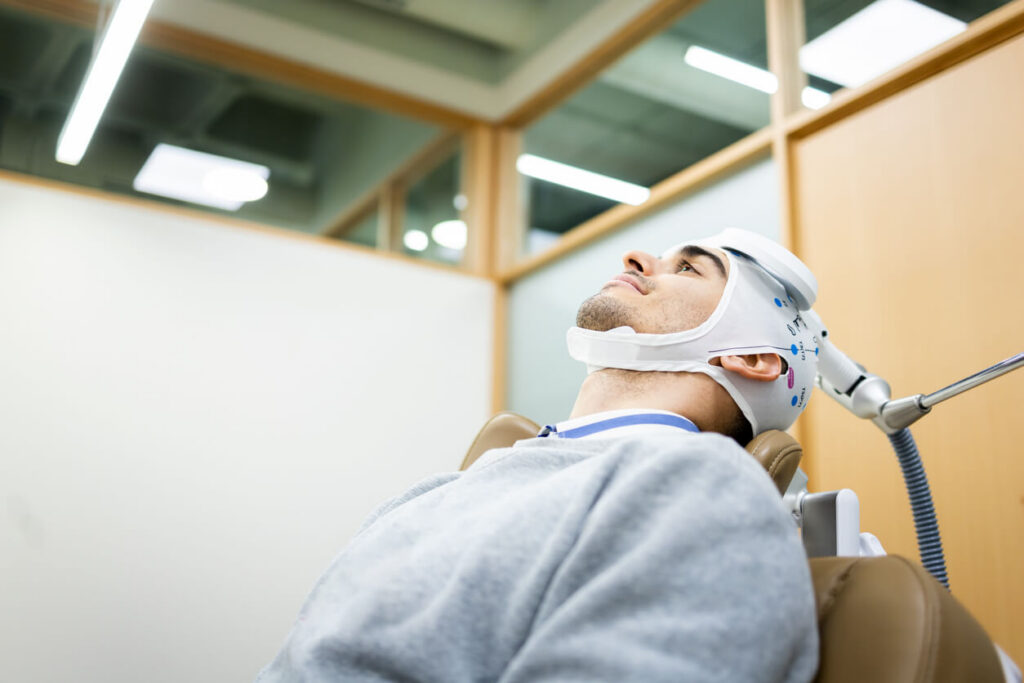
Transcranial Magnetic Stimulation (TMS) uses gentle magnetic pulses placed against the scalp to stimulate specific areas of the brain involved in mood. You stay awake and alert during the entire session. There’s no anesthesia, no sedation, and no hospital stay.
Treatment is done in an outpatient setting, and most people return to their normal activities. This includes driving right afterward, unless their provider advises otherwise.
Electroconvulsive Therapy (ECT) works differently. It uses controlled electrical currents delivered to the brain while you are under general anesthesia.
The treatment intentionally triggers a brief seizure that lasts about 30 to 60 seconds. Because anesthesia is required, ECT is performed in a hospital or surgical setting. You must fast beforehand, and you’ll need someone to drive you home afterward. Most people also need time to recover for the rest of the day.
Both treatments can reduce depression symptoms, but the overall experience, from preparation to recovery, is very different.
Why Is TMS Better Than ECT Initially (Outside of Emergencies)?
Both treatments can be effective for treatment-resistant depression. The choice often comes down to the urgency of the situation, a person’s medical history, and how treatment may affect everyday life.
When providers evaluate these options, they consider several clinical factors that can influence their recommendations.
1. Safety and Tolerability
As mentioned earlier, TMS does not require anesthesia, eliminating the risks associated with sedation.
Common side effects include:
- Scalp discomfort at the stimulation site
- Mild headaches
- Temporary facial twitching
- Lightheadedness
These effects usually lessen after the first few sessions. Seizures during TMS are considered rare.
ECT is associated with more substantial side effects:
- Short-term confusion and autobiographical memory loss (very common)
- Difficulty learning new information
- Headaches, muscle aches, nausea
- Anesthesia-related risks
- Some individuals report persistent memory deficits
ECT often causes memory-related side effects. The severity can vary depending on the technique used (such as unilateral versus bilateral electrode placement) and individual patient factors.
Many patients experience some loss of autobiographical memory for events that occurred during or around the treatment period. Because muscle relaxants are used during the procedure, it’s also common to have temporary muscle soreness afterward.
2. Treatment Experience and Daily Function
TMS sessions take place in an outpatient setting. You can drive yourself to appointments and typically return to work or regular activities the same day. Since you remain conscious throughout, there’s no recovery period needed. This makes TMS particularly appealing for those who need to maintain daily responsibilities.
ECT requires fasting before each session, hospital-based administration, post-treatment recovery, and arranged transportation. Most people need to take the remainder of the day off, making ECT even more disruptive to daily routines. The risks associated with repeated anesthesia also factor into many patients’ decisions.
3. Precision and Personalization
TMS is designed to focus on specific brain regions involved in mood regulation. Treatment parameters can be adjusted to individual needs, and the magnetic coil is carefully positioned over the targeted areas. In some specialized settings, functional MRI may be used to help guide stimulation based on brain connectivity patterns, though this approach is not routine in most clinics.
ECT, by contrast, affects the brain more broadly. Because it produces a generalized seizure, its effects are not limited to one specific region. While this wider impact may enhance its effectiveness in severe cases, it also means there is less ability to tailor stimulation to specific neural circuits. It also has a higher likelihood of more widespread side effects.
TMS Treatment vs. ECT for Depression
Many people ask, “Is TMS more effective than ECT?”
The answer depends on symptom severity, urgency, medical history, and personal priorities. In non-emergency cases, providers often recommend TMS first because it is less invasive and carries fewer cognitive risks.
TMS may be considered when you:
- Have moderate to severe depression that hasn’t improved with medication and talk therapy
- Want to reduce the risk of cognitive side effects, including memory problems
- Need to continue working or managing daily responsibilities during treatment
- Prefer a non-invasive option that does not require anesthesia
- Have experienced difficult or intolerable medication side effects
- Are looking for a treatment with a lower overall medical risk profile
Research suggests that TMS is associated with response rates of approximately 50–60% and remission rates of 30–35% in treatment-resistant depression.
ECT may be more appropriate when:
- Severe depression includes acute suicidal thoughts or behaviors requiring urgent intervention
- Psychotic features are present
- Catatonia is involved
- Previous treatments, including TMS, have not provided sufficient relief
- The severity of symptoms outweighs concerns about side effects
- Rapid symptom reduction is critical in a psychiatric emergency
ECT remains one of the most effective acute treatments for severe depression. Studies report response rates of around 73% and remission rates of nearly 51% in moderate-to-severe cases. Meta-analyses also show that ECT can be particularly effective in patients with psychotic depression and in older adults.
These response and remission rates show how many people experience meaningful improvement or near-complete symptom relief with each treatment.
In general, higher percentages suggest a greater likelihood that patients will see significant reductions in depression symptoms. However, note that individual results can vary.
Side Effects of TMS vs. ECT
| Category | TMS (Transcranial Magnetic Stimulation) | ECT (Electroconvulsive Therapy) |
| Anesthesia Required? | No anesthesia or sedation required | Requires general anesthesia |
| Common Physical Effects |
|
|
| Cognitive Effects | No significant memory loss was reported in most patients |
|
| Seizure Risk | Very rare when guidelines are followed | A seizure is intentionally induced as part of the treatment |
| Recovery Time |
|
|
| Impact on Daily Routine |
|
More disruptive due to fasting, anesthesia, and recovery requirements |
Treatment Schedules and Time Commitment
Understanding the time commitment helps you plan around your responsibilities.
Standard TMS Protocol
- 20-36 total sessions
- Five sessions weekly for 4-6 weeks
- Sessions range from 3-40 minutes, depending on protocol
- Outpatient office setting
- No preparation or recovery time required
- You can typically drive yourself and return to activities
Accelerated TMS protocols condense this timeline substantially, delivering care over shorter periods with multiple daily sessions.
ECT Protocol
- 6-12 total sessions
- Two to three sessions weekly for 3-4 weeks
- Approximately 60 minutes per session, including preparation and recovery
- Hospital-based administration
- Fasting required beforehand
- Transportation assistance needed
- Recovery time typically requires the remainder of the day off
For individuals maintaining employment or family responsibilities, TMS scheduling integrates more easily into daily routines.
Treatment Sequencing Options
TMS and ECT are not mutually exclusive choices. Understanding how they can work together provides flexibility.
Some individuals initially try ECT due to symptom severity or a provider’s recommendation, then transition to TMS for maintenance or if ECT side effects become problematic. Since these work through different mechanisms, responses to one do not predict responses to the other.
Conversely, if TMS provides insufficient symptom relief, ECT remains available. Many psychiatrists view this as a logical progression: optimize medication management, then TMS, reserving ECT for situations where other approaches have not succeeded.
FDA-Cleared Uses of TMS
FDA-cleared uses of TMS vary by device and protocol. Examples include:
- Repetitive TMS for major depressive disorder in adults who have failed to achieve satisfactory improvement from prior antidepressant medication
- rTMS as adjunct treatment for MDD in adolescents ages 15-21
- Deep TMS for obsessive-compulsive disorder as an adjunct treatment
- Specific TMS systems cleared as an aid in short-term smoking cessation
- Certain TMS devices for the acute treatment of migraine with aura
Research is ongoing for PTSD, bipolar depression, and other mental health conditions, though these remain off-label applications.
Start Your Journey to Recovery With Expert TMS Treatment
Serenity Mental Health Centers was founded in 2017 to provide more effective treatment options for depression, anxiety, and other mental health conditions. Today, our growing network of clinics across the United States continues that mission by offering personalized, science-based care tailored to each individual.
TMS therapy is one of our signature treatment options. As a medication-free, outpatient procedure, it allows you to continue your normal activities without hospital stays, anesthesia, or extended recovery time.
At Serenity, you’ll work closely with a dedicated psychiatrist who takes the time to understand your unique needs and create a treatment plan designed specifically for you. We’re committed to providing compassionate, research-backed care that helps you move forward with confidence.
Ready to explore whether TMS is right for you? Request an appointment today or call to speak with our team about your options.